Reliability of Ultrasound in Detecting Cartilage Change in Patients with Rheumatoid Arthritis: A Study By Omeract Ultrasound Task Force
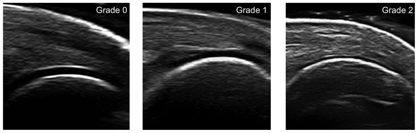
Tenosynovitis US scoring systems follow synovitis and clinical scoring systems in RA and are responsive to change after biologic therapy
Ultrasound-detected tenosynovitis independently associates with patient-reported flare in patients with rheumatoid arthritis in clinical remission: results from the observational study STARTER of the Italian Society for Rheumatology
Tenosynovitis on Ultrasound: Common in RA Remission
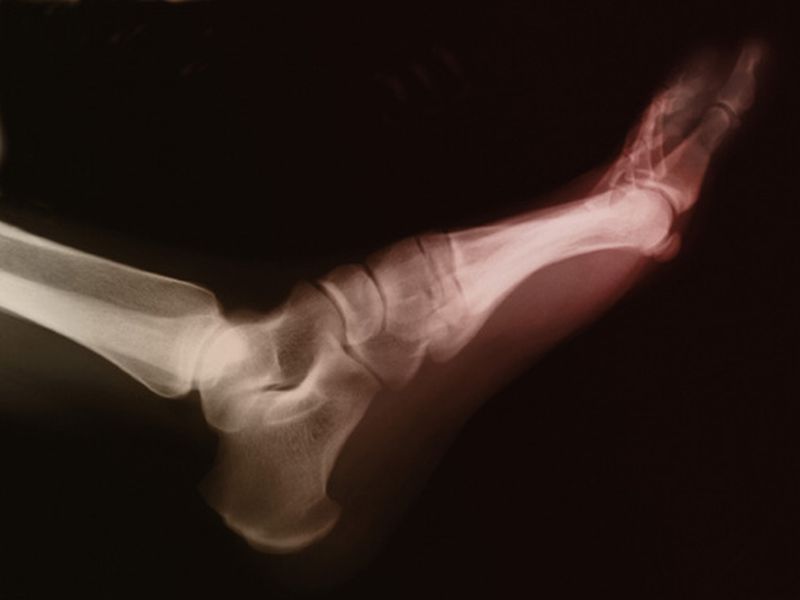
“Patients with SpA and gout more often had tibiotalar joint synovitis. The RA group more often had tibialis posterior (TP) tenosynovitis than other groups. Compared with the other groups, the early RA group more often had subtalar and talonavicular joint synovitis.”
Ultrasound in Rheumatology finds its widest and best evidenced application in Rheumatoid Arthritis. Grading scales for synovitis, tenosynovitis and bone erosions have been validated, and inter-rater reliability well-documented.
Its applications in RA include:
1) early diagnosis of inflammation even before patients fulfil current classification/diagnostic criteria for RA, thus allowing for earlier effective treatment to be instituted;
2) assessing rapid resolution of inflammation in response to various fast-acting but costly targeted therapies, allowing for timely therapeutic switches should the selected agent prove ineffective;
3) monitoring and guiding treatment intensity in accordance to current treat-to-remission-target strategies, in the realistic hope of preventing irreversible damage & disability, and in quickly restoring function and quality of life;
4) advising whether patients in sustained clinical remission can safely taper down and off their therapies;
5) monitoring and detecting disease flares, so as to rapidly and fully re-induce remission.
There is now a good body of evidence for the use of ultrasound in all these decision milestones in modern RA management, more than enough to categorically state that point-of-care ultrasound is indispensable to modern Rheumatology practice. Only point (3) remains controversial, but I’m sure I can convince you in the coming days on why I believe MSUS will even win the day on this.


